Posters presented in 2019
Presented at MAR Conference, October 2019
(click image to view poster)
"Impact of a Standardizing Approach to Turning and Repositioning Patients at Risk for Pressure Injury Development"
Liz Stehr, BSN, RN, CWOCN & Judy Stasuk, MSN, RN, CWOCN, CFCN
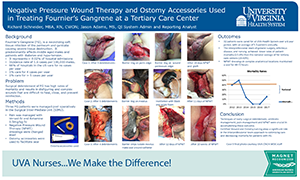
Posters presented in 2018
Presented at SAWC 2018 Spring in Charlotte, NC
(click image to view poster)
Abstracts (WOCN® Conference, May 2017)
Wound—Product Selection and Innovations
CS02
INSTILLATION THERAPY AND ITS EFFECTS ON WOUND HEALING
Deanna Zaganas, BSN, RN, WOC, , and Dana Balassa, BSN, RN, WOC, , Glen Burnie, MD
FACILITY: An acute care hospital in the Northeastern United States. CLINICAL PROBLEM: Equipment was available at our facility, but it was not being utilized. We wanted to see if using the instillation* therapy would make a difference in our patient's wound healing. CLINICAL APPROACH: First, it was necessary to get the approval of a few surgeons who would allow us to use instillation* therapy on their patients. After the surgeons agreed on its use on their patients, the inpatient nursing staff had to be educated on how to monitor and/or troubleshoot the instillation* treatment process while they were taking care of a patient receiving this instillation* therapy. Three patients were selected for this case study, and serial pictures were taken at different intervals of their treatment. OUTCOME: The surgeons were happy with the appearance of their patients' wounds when the therapy dressings were changed. The instillation* therapy jump-started the healing process and therefore made the patients happier. The instillation and dwelling of approved fluids avoided the need for the patient to return to the operating room (OR) for washouts with dressing changes. CONCLUSION: Instillation* therapy was effective in jump-starting the wound-healing process and successfully promoted faster healing time while in an inpatient setting. It reduced the surgical risks to these patients by avoiding the need to return to the OR under anesthesia.
http://http://www.acelity.com/products/tech/vera-flo-therapy. Published 2014.
http://http://www.acelity.com/products/vac-veraflo-dressings. Published 2014.
http://http://www.veraflo.com/about-v-a-c-veraflo-therapy. Published 2016.
Kim P, Attinger C, Crist B. Negative pressure wound therapy with installation: review of evidence and recommendations. Wounds. 2015;27(12):1–20.
Kim P, Attinger C, Steinberg J, et al The impact of negative pressure wound therapy with instillation compared with standard negative-pressure wound therapy: a retrospective, historical, cohort, controlled study. Plast Reconstr Surg. 2014;133:709–716. View Full Text | PubMed | CrossRef
Wound—Product Selection and Innovations
CS05
A SWEET SOLUTION: THE USE OF MEDICAL-GRADE HONEY ON ORAL MUCOSITIS IN THE PEDIATRIC ONCOLOGY PATIENT
Ferne Elsass, MSN, RN, CPN, CWON, , Norfolk, VA
PROBLEM: Pediatric patients develop mucositis when receiving treatments such as chemotherapy and radiation. The gastrointestinal mucosa's epithelial cells divide quickly, leading to breakdown and painful ulceration. The most common and sensitive is oral mucositis. Patients developed painful bleeding ulceration and thick mucoid saliva. Lips eventually crack and bleed. Mouth rinses containing antimicrobial, antihistamine, and analgesic medications are the mainstay for pediatric patients. These rinses are often refused related to taste or texture. Patients less than a year old are unable to use these products. Continued oral mucositis leads to increased pain and refusal or inability to eat. PROJECT OBJECTIVE: Outcomes from oral mucositis such as decreases in nutritional intake and deteriorating oral hygiene developed from the painful, bleeding ulcers and dry crusting of the mouth. Alternatives to standard treatments were necessary. Leptospermum honey was added to daily mouth care. At completion of this poster, this treatment has been used in 10 pediatric oncology patients between the ages of 9 months and 17 years. CASE SERIES: To demonstrate the improvement of oral mucositis with standard oral care and the additional use of active Leptospermum honey in 3 pediatric oncology patients. OUTCOME: The Leptospermum honey paste was easy to apply and well received by all patients. The patient received oral care every 4 hours, followed by the application of the honey paste 2 to 3 times daily. The paste was applied with a sponge swab, coating the mouth. Patients either swished and spit or had excess suctioned out. Three selected examples of the 10 patients are presented in the poster. Leptospermum honey paste proved to be effective in all participating patients. Healing observed within 3 days, and patients in all cases reported decreases in pain. Decrease in wounds and bleeding was evident in all cases within 5 days.
1. Miller M, Donald D, Hagemann T. Prevention, treatment of oral mucositis in children with cancer. J Pediatr Pharmacol Ther. 2012;17(4):340–350. PubMed
2. Molan P, Rhodes T. Honey: a biologic wound dressing. Wounds. 2015;27(6):141–151. PubMed
3. Rashad U, Al-Gezawy S, El-Gezawy E, Azzaz A. Honey as topical prophylaxis against radiochemotherapy-induced mucositis in head and neck cancer. J Laryngol Otol. 2009;123:223–228. doi:10.1017/S0022215108002478. PubMed | CrossRef
4. Song J, Twumasi-Ankrah P, Salcido R. Systematic review and meta-analysis on the use of honey to protect from the effects of radiation-induced oral mucositis. Adv Wound Care. 2012;25(1):23–28.